Nitrofurans: Niridazole and other antibiotics
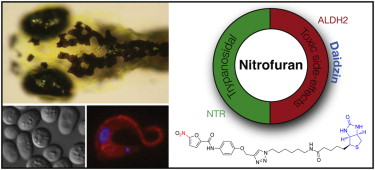
Nitrofurans
Niridazole
Niridazole is a nitrothiazole derivative related to metronidazole and is widely used in some countries for the treatment of schistosomiasis. In rodent species, it has been found to affect spermatogenesis during meiosis.
A study of 25 men with bilharzia in Egypt showed that a 10 day course of treatment depressed semen volume and sperm count and motility 1 week after cessation of treatment. This persisted 3 months after treatment was discontinued. Testicular biopsy at 1 week in eight men showed focal germinal cell hypoplasia and/or spermatocyte arrest. At 3 months, repeat testicular biopsy in these men showed normal spermatogenesis in six but persistant abnormalities in the remaining two subjects.
Nitrofurantoin
Early studies in rats showed that nitrofurans including nitrofurantoin produced transient spermatogenic arrest at the stage of the primary spermatocyte. In a clinical study performed in 1956 (and unlikely to be repeated) prisoners and medical student ‘volunteers’ were given a 14 day course of nitrofurantoin at a daily dose of lOmg/kg. Semen samples were obtained pre- and post-treatment. Testicular biopsies were performed pre- and posttreatment in one third of medical students and all prisoners! The results were difficult to interpret. The majority of volunteers showed no changes in sperm count or testicular histology. In approximately 30% of the subjects a temporary decrease was recorded in sperm count but without accompanying histological abnormalities.
The recommended daily dose of nitrofurantoin is now approximately 5 mg/kg and this compound is sometimes used for long-term antibiotic therapy. No clinical studies have reported an adverse fertility effect at this dose, but Schlegel and co-workers recommend avoidance of nitrofurantoin as long-term suppressive therapy in men ‘interested in fertility’. Certainly if a man has a suboptimal semen analysis on nitrofurantoin, withdrawal of therapy would be a sensible first-line measure.
Ketoconazole
The data sheet for the antifungal drug ketoconazole notes that gynaecomastia and oligospermia have been reported in rare instances. A possible explanation for this can be provided from a study performed in five healthy volunteers who each received a single oral dose of 400 mg of ketoconazole. The levels of total and free testosterone fell sharply, reaching a nadir of approximately 30% below baseline levels within 4 to 6 hours of drug ingestion.
The decrease was thought to be caused by reduced testosterone synthesis as it is known that spermatogenesis is regulated by intratesticular levels of testosterone. The authors state that this mechanism could be responsible for the loss of libido and potency seen in men on ketoconazole, although no data are provided on the incidence of these sexual dysfunctions. Furthermore, the drug manufacturers acknowledge the transient fall in testosterone levels in the data sheet but note that during long-term therapy testosterone levels are not usually significantly different from controls.
Tetracyclines
Tetracyclines do not appear to affect spermatogenesis, but some forms may have a direct toxic effect on mature sperm. Chlortetracycline has deleterious effects on human sperm at concentrations of 100 mg/1 and minocycline has been found to be toxic to bull sperm. Tetracycline hydrochloride is not toxic to ejaculated human sperm at concentrations of 4ug/106 sperm, but it has not been tested at higher concentrations.
Schlegel et al., (1991) suggest that when these drugs are used to treat genito urinary infections any adverse effect may be outweighed by the beneficial effect of eradicating infection and inflammatory cells from the ejaculate. In men requiring long-term antibiotic administration, the type of antibiotic should be judiciously chosen. However, it must be noted that the few studies published that do demonstrate sperm toxicity with tetracyclines were performed between 1955 and 1975 and no recent evidence substantiates toxic effects in humans at therapeutic doses.
Demeclocycline
A single case report describes a 22-year-old man who, after several years of treatment with tetracycline for acne, changed to demeclocycline. He complained of decreased libido at doses between 300 to 600mg/day. The symptoms resolved within a week of discontinuing the drug.
Macrolides
The macrolides, which include erythromycin and spiramycin, have no effect on human or animal sperm at long-term exposure to therapeutic drug concentrations. However short-term exposure at high doses may impair sperm motility. Erythromycin administered at therapeutic levels decreased the frequency of mitotic division in rat testes. Based on this data, Schlegel et al (1991) suggest that macrolides might impair fertility in men during the period of drug administration.