7 Little-Known Facts about Antibiotics
Antibiotics are powerful drugs that cure disease by damaging or killing bacteria. Penicillin, the first antibiotic, was serendipitously discovered from a mold culture in 1928. Today, hundreds of different antibiotics are applied in clinical practice to cure both minor and severe infections. Before you start taking antibiotics, there are several fundamentals you need to know about them that are not directly stated in medication guide.
Antibiotics May Disrupt Your Gut Microbiome
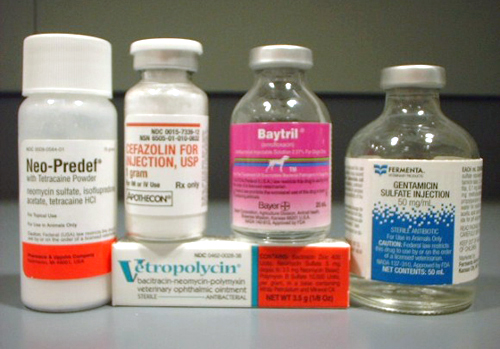
Antibiotics usually disrupt human intestinal metabolism by injuring beneficial bacteria of gut microbiota – an ecosystem of trillions of microorganisms populating the gastrointestinal tract that ensure proper food digestion and detoxification. Some 10% of those bacteria are toxin-producing pathogen species, while 90% are beneficial species.
When entering the gastrointestinal tract, antibiotics tend to destroy the beneficial bacteria, thus causing imbalance of “good” and “bad” microorganisms – a condition called dysbiosis. The symptoms of dysbiosis include intestinal pain, bloating, gas, constipation and/or diarrhea. To restore the balance, a patient is advised to start taking probiotics – food supplements containing two most beneficial bacteria Lactobacillus acidophilus and Bifidobacterium bifidum – immediately after finishing antibiotics treatment. It takes at least 40 days to restore the normal flora of the gut with probiotics therapy to avoid long-term gastrointestinal health problems.
Antibiotics May Cause Fungi Infections
Candida (fungi) is one of the 10% of “opportunistic pathogens” that harmlessly colonize the human digestive tract. However, when the balance is upset after antibiotic treatment, candida can proliferate causing fungal infections such as vaginitis in women, fungal infections of the skin, oral candidiasis. When a fungal infection enters systemic circulation, it may cause systemic candidiasis whose consequences can be lethal. Consult with your practitioner on the best anti-fungal drugs if you spot the first symptoms of fungi infection. An anti-fungal diet consists mostly of protein and complex carbohydrates and calls for avoidance of concentrated sweets and sugar.
Antibiotics Don’t Cure Viral Infections
Take antibiotics only when you get a bacterial infection such as bacterial pneumonia, strep throat and E. coli urinary tract infections. Antibiotics don’t cure viral infections such as flu, colds, runny nose, most coughs and bronchitis, most sore throats, many ear infections. Taking antibiotics when you do not need them boosts the risk of getting an antibiotic-resistant infection later.
Bacteria Getting Immune to Antibiotics
One of the principal concerns in contemporary medicine is antibiotic resistance. In simple terms, when an antibiotic is used frequently or too long, bacteria become immune or develop resistance to that antibiotic. Some of today`s infections are caused by bacteria resistant to some antibiotics. This creates the danger of life-threatening infections that cannot be cured at all, e.g. some varieties of incurable tuberculosis among prisoners.
Antibiotic Generation Matters
There are several – at least five – generations of antibiotics. Some older-generation antibiotics of tetracycline group have almost lost their effectiveness against many modern infections. Some newest-generation antibiotics are capable to overcome antibiotic resistance in bacteria that secrete β-lactamase which otherwise disables most penicillins. Clavulanic acid, sulbactam and tazobactam are the most popular β-Lactamase inhibitors added to modern antibiotics such as amoxicillin, ticarcillin and others to help them fight the new bacterial infections. It is better to purchase generic versions of such medications from a Canadian pharmacy website to save yourself some money.
Race Against Time to Create New Antibiotics
As antibiotic resistance proliferates, healthcare officials and scientists race time or even against time. Creating new generations of antibiotics remains mostly a matter of chance: pharmacists test millions of molecules on live bacteria or enzymes and look for proof of inhibitory effects. It takes at least 10 years and a billion dollars to develop a new drug and bring it to market. In the meanwhile, bacteria develop resistance to new drugs just as fast and even faster. There is a growing concern that, given current state of research, in the next 50 years, humankind may return to pre-penicillin era when antibiotics will lose their capabilities in fighting increasingly resistant bacteria.
Nanotechnology to the Rescue
In recent years, encapsulation of antibiotics in nano granules has materialized as the most promising drug delivery technology that can transport the drug exactly to infectious cells and release it in a targeted and controlled manner boosting the drug`s efficiency. While most of nanoparticle-based antibacterial drug delivery systems are still in preclinical development, several have been approved for use in clinical practice and they look increasingly promising in overcoming antibiotic resistance.